 |
 |
|
|
Renewing the
Commitment:
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
Title I Funding in California by EMA (in millions) | ||
| FY 1997 | FY 1998 | |
| Los Angeles |
$30.4 |
$30.6 |
| Oakland (Alameda/Contra Costa) |
$6.0 |
$5.9 |
| Orange County |
$4.1 |
$3.8 |
| Riverside/San Bernardino |
$5.7 |
$5.6 |
| Sacramento (includes El Dorado and Placer) |
$2.5 |
$2.4 |
| San Diego |
$8.3 |
$8.5 |
| San Francisco (includes San Mateo and Marin) |
$37.7 |
$36.4 |
| San Jose (Santa Clara) |
$2.4 |
$2.4 |
| Santa Rosa (Sonoma) |
$1.2 |
$1.2 |
| Total California Title I Funds |
$98.3 |
$96.8 |
In California, over 90% of people living with AIDS reside in one of the states nine Title I EMAs, including: Los Angeles, Oakland, Orange County, Riverside/San Bernardino, Sacramento, San Diego, San Francisco, San Jose and Santa Rosa.
Under the law, each Title I area is required to establish a planning council, comprised of public health officials, community-based service providers, and people living with and affected by HIV/AIDS, among others. The planning council model was designed to ensure responsive, community-driven planning at the local level, and has become a model for other health programs, including HIV prevention. Given the new and constantly changing HIV treatment environment, this local flexibility will remain critical.
Dramatic drops in AIDS deaths and the resulting increase in people living with HIV/AIDS means that in the coming year more individuals will depend on Title I-funded programs for medical care and support services. Reports of successful HIV treatments are encouraging many individuals living with HIV, even those who were previously quite wary of the public health system, to address their long neglected health care needs. The complexity of new anti-HIV regimens has also increased the costs of providing highly sensitive diagnostic tests to clients. As a result of these trends, Title I resources must be expanded in FY 1999 in order to maintain and expand access to critical medical and support services.
Title II of the CARE Act provides grants to all states, the District of Columbia and the U.S. territories to provide medical and support services for people living with HIV, including HIV-related drug therapies through the AIDS Drug Assistance Program (ADAP). State health departments administer Title II grants, with community involvement in many states through local planning bodies known as consortia. In FY 1998, California will receive $30.6 million in Title II service funding and over $43 million in ADAP funding.
The advent of costly, yet promising combination therapies (which cost
between $12,000 to $20,000 per year per individual) will continue to heighten the
importance of the ADAP program, which in many cases is the only source of
subsidized drugs for uninsured, non-Medicaid eligible individuals. Recent
federal HIV treatment guidelines (see box) set a new standard for the
treatment and monitoring of HIV disease, and specifically addressed the
use of combination therapy (i.e., the use of at least three antiviral
drugs, including one of the potent protease inhibitor drugs).
Unfortunately, because of insufficient ADAP funding, many states
throughout the country have been unable to meet these standards
consistently. A July 1997 report by the National Alliance of State and
Territorial AIDS Directors and the AIDS Treatment Data Network found that
35 states had implemented at least one emergency measure because of lack
of ADAP funding, including capping enrollment to the program and reducing
the number of drugs covered. Fortunately, California has not had to impose
such harsh programmatic restrictions, primarily because of its substantial
state contribution to ADAP. In FY 1999, increased federal funding for ADAP
will be essential to preventing similar crises in California and other
states.
$12,000 to $20,000 per year per individual) will continue to heighten the
importance of the ADAP program, which in many cases is the only source of
subsidized drugs for uninsured, non-Medicaid eligible individuals. Recent
federal HIV treatment guidelines (see box) set a new standard for the
treatment and monitoring of HIV disease, and specifically addressed the
use of combination therapy (i.e., the use of at least three antiviral
drugs, including one of the potent protease inhibitor drugs).
Unfortunately, because of insufficient ADAP funding, many states
throughout the country have been unable to meet these standards
consistently. A July 1997 report by the National Alliance of State and
Territorial AIDS Directors and the AIDS Treatment Data Network found that
35 states had implemented at least one emergency measure because of lack
of ADAP funding, including capping enrollment to the program and reducing
the number of drugs covered. Fortunately, California has not had to impose
such harsh programmatic restrictions, primarily because of its substantial
state contribution to ADAP. In FY 1999, increased federal funding for ADAP
will be essential to preventing similar crises in California and other
states.
Title III of the CARE Act provides direct federal grants for HIV-related medical, pharmaceutical and support services through public and private community-based clinics nationwide. Because these clinics are often non-AIDS specific and provide health care in underserved and/or remote communities, they have a unique opportunity to identify HIV disease early and intervene prior to the onset of symptoms. While most Title III grantees are located in the urban epicenters, Title III grants are increasingly targeted to more rural, isolated areas in an effort to address the expanding epidemic. In 1997 there were 20 Title III programs in California, including programs in Bakersfield, Compton, Guerneville, Long Beach, Los Angeles, Oakland, Panorama City, San Bernardino, San Diego, San Francisco, San Jose, San Marcos, Santa Ana, Santa Barbara, Santa Cruz, Stockton, and Ukiah. Increased Title III funding in FY 1999 will expand access to HIV-related medical, pharmaceutical and support services.
Title IV of the CARE Act provides grants for services and clinical research programs for infants, youth, young adults and their families. Health care providers that focus on care to adults often have difficulty including youth-focused messages and programs in their service systems. Thus, programs and initiatives that focus on the needs of youth, such as those supported by Title IV, are essential to early intervention efforts. There are four Title IV programs in California, each of which funds a number of pediatric and/or youth services. Nationally, Title IV funds 330 sites in 27 states, many based within maternal and child health programs. Funding maternal and child health programs will remain important because of the recent successes in the reduction of perinatal transmission of HIV through the use of AZT during pregnancy and delivery.
Title V of the CARE Act includes three discrete programs: Special Projects of National Significance (SPNS), the HIV Dental Reimbursement Program, and the AIDS Education and Training Centers (AETCs). SPNS provides multi-year funding to innovative or model programs, including the Native American HIV Projects. SPNS programs are funded through a percentage contribution from other CARE Act titles, which is capped by statute at $25 million. The HIV Dental Reimbursement Program supports the provision of dental and orthodontic care for people living with HIV/AIDS through university-based dental schools. Oral manifestations of HIV disease are often the first to appear, providing an excellent opportunity for early diagnosis and treatment. In addition, poor dental health often contributes to systemic infections, malnutrition, and the malabsorption of anti-HIV drugs, which can lead to drug resistance. Finally, the AETCs provide HIV-related education and continued training to health care professionals throughout the United States. The availability of this training is particularly important given the varying perspectives on what constitutes an appropriate standard of HIV clinical care and the rapidly changing developments in HIV-related clinical research.
|
FY 1998 |
FY 1999 Community Need |
Increase | |
| Title I |
$464.8 |
$570.0 |
$105.2 |
| Title II |
$257.0 |
$342.0 |
$85.0 |
| ADAP |
$285.0 |
$458.0 |
$173.0 |
| Title III |
$76.3 |
$113.0 |
$36.7 |
| Title IV |
$41.0 |
$65.0 |
$24.0 |
| Dental |
$7.8 |
$9.0 |
$1.2 |
| AETCs |
$17.3 |
$24.3 |
$7.0 |
| TOTAL |
$1,149.2 |
$1,581.3 |
$432.1 |
The most notable Department of Housing and Urban Development (HUD) program that serves people living with HIV/AIDS is Housing Opportunities for People With AIDS (HOPWA). HOPWA-funded programs assist individuals living with HIV/AIDS who have extremely limited financial resources. According to a March 1997 General Accounting Office (GAO) report, about 70% of HOPWA clients have incomes below $500 per month.
As with the CARE Act, the cornerstone of HOPWA is its flexibility, which allows states and local communities to develop a range of housing services based on the locally identified needs of people living with HIV/AIDS.
HOPWA funds are distributed through both formula-based (90%) and competitive grants (10%). To receive HOPWA formula-funding, a jurisdiction must have reported at least 1,500 AIDS cases (since 1981) and have a population of at least 500,000. In FY 1998, $183.6 million was distributed through formula grants to 59 eligible metropolitan statistical areas (EMSAs) and 29 eligible states. The remaining ten percent will be awarded competitively in the coming months.
HOPWA Formula
Funding in California* | ||
| FY 1997 | FY 1998 | |
| State of California |
$1.9 |
$2.3 |
| Los Angeles |
$10.1 |
$10.1 |
| Oakland |
$1.6 |
$1.6 |
| Riverside-San Bernardino |
$1.2 |
$1.3 |
| Sacramento |
$.6 |
$.6 |
| San Diego |
$2.1 |
$2.1 |
| San Francisco |
$9.4 |
$8.5 |
| San Jose |
$.6 |
$.6 |
| Santa Ana |
$1.1 |
$1.1 |
| Formula Fund Total |
$ 28.6 |
$28.2 |
* These funds do not include competitive grants received by individual community-based organizations in the state
In San Francisco, HOPWA funds support a range of housing programs, including rental subsidies and capital development. In addition to the City and County of San Francisco, eight other California cities and the state are eligible for HOPWA funding.
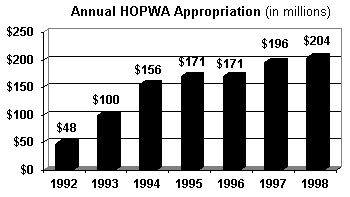
Unfortunately, federal HOPWA funds have not kept pace with the growing need for HIV/AIDS housing services. Of particular concern to AIDS advocates is the fact that the number of localities eligible for formula grants increases by 8-10 each year, while the annual federal appropriation has not grown at the same rate. As a result, a number of jurisdictions, including San Francisco, have experienced decreases in annual HOPWA formula grants in recent years, despite increasing numbers of individuals living with HIV/AIDS in need of housing support.
In addition to HOPWA, the McKinney/Homeless Assistance Grants (HAG) serve as a key federal resource in efforts to stabilize the lives of homeless individuals living with HIV/AIDS, and in doing so, facilitate access to appropriate medical care and treatment. From 1993 to 1995, McKinney/HAG funding doubled from $572 million to $1.1 billion. In FY 1996, McKinney/HAG funding was cut by 25% to $823 million, where it has remained for three years. Restoration and expansion of McKinney/HAG funding would create additional low-income housing slots for homeless individuals and families, including those with HIV disease.
The twenty-four institutes of the National Institutes of Health (NIH) are the primary sources of government sponsored biomedical research in the United States. Advances in societys knowledge about the virology and pathogenesis of HIV have been driven largely by the public/private partnership between NIH and the pharmaceutical industry. Recently, Administration officials and Congressional leaders announced their intent to double the NIH budget over the next five years to enhance the nations research efforts. SFAF applauds this expanded commitment to research, with the understanding that this expansion must not come at the expense of other important HIV/AIDS and health programs.
The NIH Office of AIDS Research (OAR) was established in 1993 to coordinate and target resources in the national HIV research effort. Since its inception, the OAR has been under assault by those who believe that targeting research funds to a particular disease is counter-productive to the overall research effort. While it is true that basic biomedical research is an essential building block for all scientific advances, targeted research efforts are also essential, particularly if we are to stem the worldwide pandemic and develop new, more powerful and more easily administered HIV treatments.
In 1997, President Clinton called
for an aggressive plan to develop an effective HIV vaccine within ten
years. SFAF agrees that a vaccine is the only hope of significantly
reducing the six million new infections now occurring annually
worldwide. The appointment of Nobel laureate Dr. David Baltimore as
the Director of the new vaccine research effort at the NIH is a clear signal of the Clinton Administrations commitment to this effort. In
addition, it is important that more research be conducted to develop
effective agents, such as microbicides, that women control (i.e., methods
other than condoms) to protect themselves from HIV infection through
sexual contact.
clear signal of the Clinton Administrations commitment to this effort. In
addition, it is important that more research be conducted to develop
effective agents, such as microbicides, that women control (i.e., methods
other than condoms) to protect themselves from HIV infection through
sexual contact.
In FY 1998, HIV/AIDS research at the NIH is funded at $1.608 billion. The scientific professional judgement request for FY 1999 is a 15% increase in the NIH budget overall, which should provide a 15% increase for HIV/AIDS-specific research as well. This 15% increase to the NIH would be a significant first step in the doubling of the NIH budget within the next five years.
For the first time in the history
of the epidemic, new cases and deaths from AIDS declined nationwide and in
California. These decreases are attributable to effective HIV  prevention efforts and expanded access to medical care and
anti-HIV drugs.
prevention efforts and expanded access to medical care and
anti-HIV drugs.
The Centers for Disease Control and Prevention (CDC) funds both primary and secondary HIV prevention efforts, with the goal of continuing to reduce the number of new HIV infections and protecting the public health. In FY 1998, HIV prevention programs at the CDC are funded at $634.3 million. The majority of these funds are awarded to state and local health departments, which then distribute funds to local programs, based on priorities set by local community planning bodies. These planning bodies are comprised of local public health officials, community members and researchers and are charged with the task of reviewing epidemiological and other behavioral research data in order to evaluate local prevention needs and establish priorities for the use of federal funds. Research demonstrates that effective HIV prevention efforts are those that are well-targeted, underscoring the critical role of this local planning process.
In FY 1998, for the first time, the CDC has proposed that a portion of newly appropriated HIV prevention program funds be used to support CDC administrative activities. At a time when every infection averted saves both lives and money, any decrease in federal support for community-based HIV prevention programs is unacceptable and should not be supported.
Finally, during the FY 1998 appropriations process, the House of Representatives attempted to eliminate permanently the Department of Health and Human Services (HHS) Secretary Shalalas authority to make federal funds available for needle exchange. SFAF urges Congress to maintain the Secretarys authority, as agreed to by the FY 1998 Labor/HHS Conference Committee.
Ensuring timely access to substance abuse treatment to people living with HIV/AIDS improves their quality of life and for some, stabilizes their lives so that they are able to take advantage of anti-HIV treatment regimens. For others, entering substance abuse treatment may prevent them from becoming HIV infected in the first place.
The Substance Abuse and Mental Health Services Administration (SAMHSA) distributes formula-based block grants to states for the development and implementation of substance abuse and mental health outreach and treatment programs. A two percent HIV set-aside within the block grant supports local community efforts to respond to the increasing proportion of people with HIV who also have substance abuse and mental health issues (this is also referred to as being "multi-diagnosed"). SAMHSA also distributes funds through direct grants to community based organizations through its three centers: the Center for Substance Abuse Treatment, the Center for Substance Abuse Prevention, and the Center for Mental Health Services.
SAMHSA officials estimate that in FY 1997, $65.9 million in block grant funds were spent on HIV/AIDS programs nationwide. Unfortunately, current SAMHSA reporting requirements do not provide detailed enough information to give a clear picture of exactly how these funds are used at the state and local levels. With nearly 50% of new HIV infections nationally now related to injection drug use, it will be increasingly important for SAMHSA and state and local public health officials to heighten the profile of substance abuse and mental health issues, and for federal funding to increase substantially so that those willing to enter drug treatment programs are able to do so.
Page last updated 10 February 1998
| HIV/AIDS Epidemiological Overview | Federal Appropriations | HIV/AIDS Housing |
|
|