 |
 |
|
Graduate Medical
Education Primer
American Medical
Student Association |
A typical college graduate seeking a career in medicine spends four
years at one of the 151 medical schools before receiving a medical degree.
But receiving a medical diploma isn't enough to practice medicine in the
United States. A newly graduated doctor must also commit three to eight
years for residency training. For the most part, residency or graduate
medical education, (GME), takes place in a teaching
hospital.
How much does it cost to train
a doctor? First-year residents receive stipends of about $30,000 a year,
rising to about $40,000 for residents in their seventh or eighth years.
Total direct cost of residents -including benefits, the cost of faculty
teaching, time, overhead, and so forth-average $70,000 per resident. But
if the full costs are taken into account-the higher cost of caring for a
patient in a teaching environment and of treating the sicker patients who
seek the specialized services available in teaching hospitals-the total
can reach $180,000.
Who pays for
physicians' graduate education? We all contribute toward funding graduate
medical education. The bulk of the financing comes from sources that are
exclusively public and tax-based: Medicare, Medicaid, the Department of
Defense and Veterans' Affairs, and state and local appropriations. With
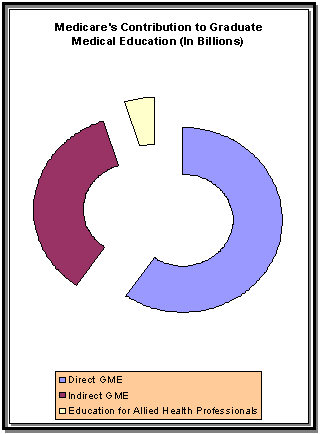
Medicare funding almost 34%--$6.4 billion-of all the GME costs. This
compensation is divided into two categories, direct GME costs (DME) and
indirect GME (IME). DME funds are intended to cover the costs of resident
salaries, supervising faculty and administrative/overhead expenses
incurred in running a residency program. $2.2 billion of the $6.2 billion
of Medicare funding is spent on DME. IME funds, on the other hand, are
intended to cover the increased operating costs generated by the presence
of residents. This is maintained by the expenditure of $3.7 billion of the
$6.2 billion. $300 million is spent on supporting graduate education for
allied health professionals.
Current Funding for
GME
 |
|
Medicare |
|
Medicaid |
|
Local & State
Appropriations |
|
Dept of Defense &
Veteran's Affairs |
Traditionally, teaching hospitals also
subsidized some of their higher costs by charging private insurance
companies more. However, in today's competitive marketplace, that is no
longer possible. Insurance companies use their market clout to ensure that
teaching hospitals are not able to charge higher rates than non-teaching
ones.
 After 30 years of
supporting graduate medical education, a number of proposals have been
introduced in order to alter GME funding by Medicare. There is currently
talk in Congress to remove GME from Medicare and subject it to the highly
politicized appropriations process. This could cause GME funding to be
vulnerable to shifts in funding from year to year due to an often partisan
appropriations process. After 30 years of
supporting graduate medical education, a number of proposals have been
introduced in order to alter GME funding by Medicare. There is currently
talk in Congress to remove GME from Medicare and subject it to the highly
politicized appropriations process. This could cause GME funding to be
vulnerable to shifts in funding from year to year due to an often partisan
appropriations process.
Fortunately,
there is a much better solution than subjecting GME funding to the
appropriations process: an 'all-payer' system. Rep. Ben Cardin (D-MD),
introduced the "All Payer Graduate Medical Education Act," HR 1224, on
March 23, 1999. The bill establishes that both public and private insurers
pay into a GME trust fund that would ease the burden on Medicare.
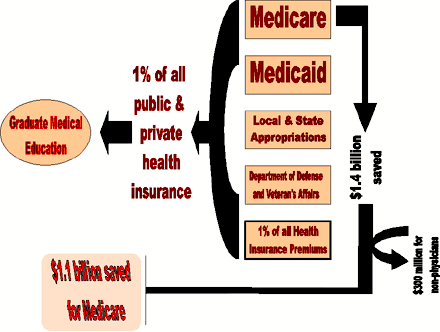
Specifically, the bill creates an
"all-payer" fund by assessing private health plans a 1% premium tax. The
estimated revenue from this health insurance tax is $3.2 billion.
Medicare, which disburses $500 billion, would pay 1% of that amount, $5
billion - $1.4 billion less than the $6.4 billion Medicare pays now. The
$300 million used by Medicare to train allied health professionals would
be removed from this process, so the overall savings to Medicare would be
$1.1 billion per year.
Proposed Funding for
GME
According to the Council of Graduate Medical Education's Fourteenth
Report (COGME), there is a current oversupply of physicians, and a skewed
distribution. Thus the bill also directs the Secretary of Health and Human
Services, in collaboration with medical community representatives, to
develop and implement a plan to reduce the number of physicians entering
residency from 129% to 110% of the number of graduates of allopathic and
osteopathic medical schools in the United States in 1993. (The rest of the
physicians who fill residency slots come from foreign medical schools.)
The ratio of generalist to specialist physicians should be increased from
the current level of 40% to 50%.
|
USMG (%) |
Total First-Year Resident
Positions |
|
140% |
24,994 |
|
130% |
23,209 |
|
120% |
21,424 |
|
110% |
19,638 |
Generalists are primary care physicians (those trained in general
internal medicine, general pediatrics, and family practice) who provide
regular, direct contact with patients, cost less than specialists and use
preventive medicine interventions daily. Currently there is a similar
provision in the Senate called the Medical Education Trust Fund Act (S.
210) introduced by Senator Moynihan.
|
Rep. Ben Cardin (H.R.
1224) |
Senator Moynihan (S.
210) |
|
1% premium tax imposed on private health
insurance |
1.5% premium tax imposed on private health
insurance |
|
129% -->110% |
|
|
50% specialist
50%
generalist |
|
Although the Moynihan bill does not contain the 50/50 and 110
provisions, it does establish an all payer trust fund. It also assesses a
1.5% premium tax on health plans in contrast to the 1% in the Cardin
plan.
Why is this issue important? The current
method of financing graduate medical education is dramatically unfair.
Managed care companies benefit from the training that residents receive in
teaching hospitals. Why should the government pay the whole cost of GME
when private industry is the primary end recipient of the
product?
However, it is important to
ensure that GME is not subjected to the wild swings of the appropriations
process. The 'all-payer' act would ensure that the training of future
physicians proceeds in a seamless
manner.
It would also ensure that quality
patient care can continue in our nation's teaching hospitals. For
instance, issues such as resident work hours ands resident safety
standards are partially determined by how much money that the hospital has
available. If funding for GME is altered, teaching hospitals may be
compelled to compromise some aspects of care in order to remain fiscally
solvent.
|
What Can You
Do?
-
Support 'all-payer'
legislation
-
Write your
representatives
-
Educate your
peers
|
- "The Doctor Track." July
1994. The Alliance for Health Reform.
- "Health Policy Report."
February 5th 1998. The New England Journal of Medicine.
- "Health Policy Forum."
Spring 1998, Vol. 3, Issue 2. The Standing Committee on Health Policy of
the American Medical Student Association.
- "COGME Physician Workforce Policies: Recent
Developments and Remaining Challenges in Meeting National Goals,
Fourteenth Report." March 1999. The Council on
Graduate Medical Education.
Written by:
Mahdi Basha, Wayne State University School of Medicine
Simon Ahtaridis, Temple University School of Medicine
1999-2000
AMSA Legislative Affairs Director
Josh Rising, Boston University School of Medicine
2000-2001 AMSA
Legislative Affairs Director |